Flashes and Floaters and Posterior Vitreous Detachment
What are flashes and floaters?
The retina is a thin layer of light sensing tissue that lines the inside of the eye – it is like the film in a camera, and allows you to see. Within the eye, the vitreous is a clear gel that fills the central part of the eyeball. It is in contact with the surface of the retina.
During development, the vitreous carries blood vessels that supply the anterior parts of the eye. Once these structures develop their own blood supply, the vessels in the vitreous disappear and it becomes clear. Retention of clarity is a primary function of the vitreous after birth, and it has no role in the maintenance of retinal attachment or eye pressure or shape.
The vitreous undergoes degenerative changes with age, and will eventually separate from the retina (‘posterior vitreous detachment’).
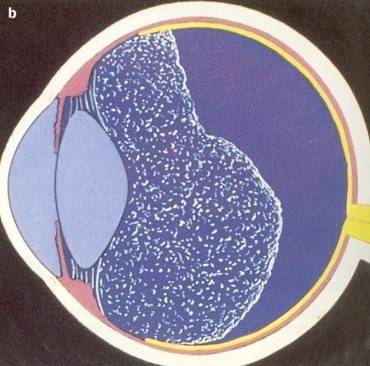
Posterior vitreous Detachment
With ageing, the vitreous gel becomes more liquid. Fibres within the gel clump together and may become visible as floaters. Eventually the vitreous pulls away from the surface of the retina and becomes mobile within the eyeball. This is known as a ‘posterior vitreous detachment’.
Floaters are opacities in the gel that are produced during this process. They are visible because they move with the newly mobile vitreous with respect to the retina. As they aren’t stationary, it is impossible for the brain to ignore them. The may be dark specks, insect-like shapes, dots, or cobwebs.
Flashes develop as the vitreous gel tugs on the retina as it separates from it. They are sparkles that are seen in the peripheral field of vision and are most often noticed in dim conditions.
The sudden onset of flashing lights and floating spots in one eye is common in people aged between 40 and 80 years. These symptoms indicate the development of a posterior vitreous detachment.
How do retinal tears and retinal detachments develop?
Separation of the vitreous gel from the retina (posterior vitreous detachment) is a normal ageing change. However, if the vitreous is abnormally attached to the retina at one point, it can pull on this point as it separates from the retina, causing the retina to tear.
A retinal tear lets fluid pass into the space under the retina, breaking down the suction that keeps the retina in its normal position. As a result the retina can lift away from the back of the eye. This is called a retinal detachment.
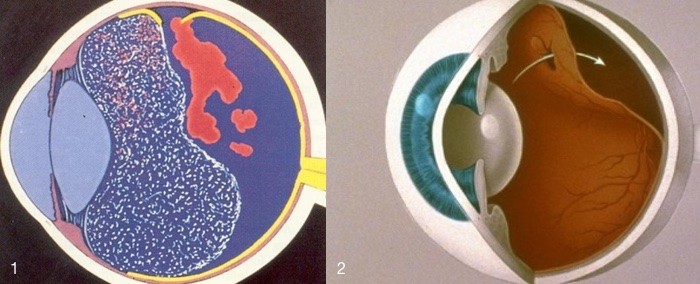
A retinal detachment causes loss of vision. The first sign of this is usually a shadow that is seen in the peripheral field of vision. This loss of vision continues until the shadow reaches the centre of the field of vision. At this stage reading vision is lost.
Without surgery, a retinal detachment will cause complete and permanent loss of vision.
What should I do if I have floaters and flashes?
If you experience the sudden onset of new flashes and floaters, it is important that an eye doctor (an ophthalmologist) examines you within a few days. This is best arranged by visiting your GP. If there is associated loss of vision ,either a shadow in the peripheral field of vision that is moving centrally, or vision is poor, then review is urgent and you should see your ophthalmologist on the same day. If your symptoms start at night, then you need to be seen the next day.
If you can’t contact your ophthalmologist, you should go to the Sydney Eye Hospital, or Prince of Wales Hospital.
What will the examination involve?
After obtaining a detailed history of your symptoms, your vision and eye pressure will be checked. Your pupils will be dilated to allow examination of the vitreous gel and the retina.
Your ophthalmologist will check to confirm the presence of a posterior vitreous detachment. Your retina will be checked carefully at the slit lamp, and the peripheral retina will then be examined whilst you are lying flat. This allows gentle indentation of the peripheral retina to ensure that any retinal tears are detected.
Treatment if no retinal tears are detected.
If no problems are detected, special follow up is not needed and no there are no special precautions. Usually, flashes and floaters become less noticeable over 4-6 weeks.
However, it is important that you return urgently if your symptoms worsen – that is, if the flashes or floaters suddenly worsen, a shadow develops in the peripheral field of vision or vision worsens. These symptoms indicate the possible development of a retinal tear or detachment.
Treatment of a retinal tear.
If a retinal tear is found, it is usually treated with laser to prevent a retinal detachment developing. Laser is usually able to be performed in the consulting rooms.
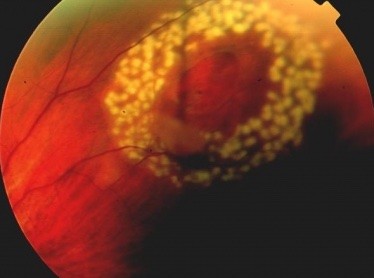
Laser treatment to a retinal tear
Laser is a bright light that is focussed on the retina and used to create a small burn in the retina and its underlying layer. Laser is applied by placing a special ‘contact lens’ on the eye, which keeps the eyelids open and the eye still, and allows your ophthalmologist to visualise the retinal tear. The laser is then used to make a ring of burns around the retinal tear. The burns heal to form a ‘weld’ that seals the tear and prevent fluid passing through the tear and spreading under the retina.
Laser is very bright and somewhat uncomfortable. However, it is safe and effective. It reduces the risk of retinal detachment from approximately to 50% to less than 4%. There are no special precautions or restrictions after laser treatment (although you can’t drive until the next day).
A check is usually arranged after 1-2 weeks.
